HOME - BLOOD - EQUIPMENT - ANATOMY - COMPLICATIONS - PREPARATION - VIDEOS - COURSE CLOSURE


Susie's Story.
Susie worked in construction up until 6 months ago. Ever since having her blood taken she has had reduced movement in her arm and has not been able to do any manual labour since.
She recalls a ‘sharp shooting pain’ sensation when she had a blood test -around the same time that the injury started.
What has happened here?


Jon's Story.
Jon went to donate blood for the first time.
As the phlebotomist entered his arm with the needle he noticed a large amount of blood seeping out around the edges.
The blood was pulsing into the collection system which was filling quickly and was bright red. Afterwards it didn’t seem to stop bleeding for ages and he was left with a huge bruise.
What has happened here?


Angela's Story.
Angela (75) had been feeling unwell for a few weeks and was not getting any better. She visited her GP who took a blood test. The lab called the GP practice the following day and said the test would need to be repeated as the sample was ‘untestable’. The GP called Angela and asked if she could come back the next day. She booked her appointment in.
Overnight Angela lost consciousness and slipped into a diabetic coma. She died of hypoglycemia. If she had got those results when she was meant to, she would have been admitted to hospital straight away and put on a treatment plan that would have saved her.
Think of EVERYTHING we have gone through so far. What kind of factors could have caused the sample to be rejected by the lab and how could it have been prevented?


Sandra's Story.
Sandra is 66. She went for a blood test as part of her annual health check.
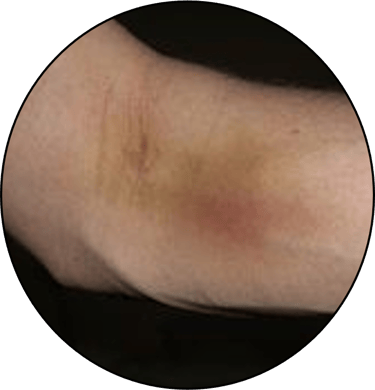
Straight after the procedure a big lump (haematoma) formed on her ACF which reduced after a few days.
For weeks after the procedure she exhibited large amounts of bruising.
How could this have been prevented? Are there any medical conditions that could have contributed?
TOP TIPS for preventing a bruise!
Tourniquet timing and tension is a delicate balance! Allow veins to fill AND drain
Apply pressure after procedure immediately and for a good amount of time (3 mins+) – and do it PROPERLY
What’s going on under that dressing? Always check the site before they leave.
Check anticoagulant use and clotting disorders
Do not insert the needle any further than you need to and KEEP ANCHORED – no wiggling! Keep an eye on that needle.
Do not apply pressure to site until needle is clear
Choose the right size needle


Simon's Story.
Simon started to feel woozy as his blood was being drawn in the GP practice. He often felt faint when having medical procedures. He was too embarrassed to say so just closed his eyes and tried to fight the feelings off.
The GP had forgotten the correct sample tube so left the room to get one mid-procedure. Meanwhile, Simon collapsed from his chair and hit his head on the sink on the way down. He was rushed to hospital with a severe head injury. An MRI scan showed he had a subdural hematoma requiring surgery.
He has suffered from the effects of brain damage ever since and has reduced mobility as a result.
How could this have gone better?
What is your experience with fainting and what do you do if it happens?
Fainting tips!!!
Always ask patients to TELL YOU if they start to feel unwell (before you start the procedure)
Ask about history of fainting - normalise it to avoid embarrassment
Know the signs and symptoms of a faint, keep an eye on your patient
Do not leave patients alone immediately after or during taking blood
Fainting can be physiological OR psychological (or both)
Check history
Apply pressure to the site and shout for help or activate alarm without leaving their side
Always keep an eye on where your sharps are
“If the patient faints during the procedure, immediately release the tourniquet, remove the needle and discard the device safely. Having the presence of mind to protect yourself from the contaminated sharp can prevent an adverse reaction from escalating into an accidental needlestick” See annex D in WHO guidelines for more info
What would happen to your patient if they fainted in YOUR clinical environment?
Do you have safe chairs/beds? Do you have a good alert system? Is your alerting method close by? What if you are community-based? Always be risk-assessing! Who do you have for support?


Preventing and dealing with needlestick incidents
KNOW your needlestick injury protocol in advance!
Have clear notices up with what do to
Report ALL exposures, however small
Seek help and PEP immediately
Prepare well for fainting and unpredictable behaviours
Do not disassemble equipment before discarding
Use safety engineered devices where available
Wear gloves (they wont stop a needle penetrating but will wipe off a lot of blood on the way in and can protect you by as much as 90%)
Have sharps bin and call bell close by
Complete training on sharps handling and incident management
Be up to date with your hepatitis B vaccines.


HOME - BLOOD - EQUIPMENT - ANATOMY - COMPLICATIONS - PREPARATION - VIDEOS - COURSE CLOSURE
